Lake Behavioral Hospital offers FREE Assessments 24/7, call us toll-free at
Frequently Asked Questions
If you have questions that are not in our FAQ’s, please call (844) 202-5555 and we will be happy to assist you.
We know patients, as well as family members, friends and referral sources have a lot of questions before, during and after inpatient treatment so we have addressed many of the frequent inquiries we receive.

What should I bring to the hospital?
Limit your clothing to what you will need in the course of a one-week stay. Casual clothing is recommended.
Three to four changes of casual clothing without drawstrings. For women, casual pants or jeans with tops or comfortable, casual dresses. For men, slacks or jeans with casual shirts. Please note that offensive or inappropriate logos will not be allowed. Laundry access is available with laundry detergent.
A supply of socks and underwear that will last between three and four days. Please do not bring tube socks or leggings.
Bring one pair of comfortable shoes without shoelaces.
A sweater or light jacket, without drawstrings.
Toiletries: Comb, brush, deodorant, toothbrush and tooth paste rechargeable electric razor. We provide toiletries, if needed. (no glass or aluminum containers, no mirrors, no alcohol content in any products, and no hair dryers or flat / curling irons)
Medications: Please bring all your medications and provide a list of your current prescription and over-the-counter medications, including dosages and frequency. SPBH will provide medications on our formulary only. This may not include medications prescribed for certain medical conditions.
Phone Numbers: Bring a list of important phone numbers, as you will not have immediate access to a cell phone while you are in treatment.
Please leave these items at home:
Please do not bring jewelry, money or other valuables. Wedding rings are appropriate.
Any clothing with drawstrings is prohibited: sweatpants, running shorts, hoodies, pajamas, shoes with shoe strings paracord jewelry or watches, etc. Belts are also not allowed on pants.
Electronic devices such as MP3 players, tablets, laptop computers, radios, cell phones, alarm clocks or other items with a cord.
Your own pillow, sheets, blanket or stuffed animal – in order to control for infections. We will supply all the linens and pillows you need during your stay.
Food and drinks from outside of the hospital. You will be provided with snacks in addition to regular meals.
All of a patient’s belongings will be searched by a qualified staff member and recorded on a Patient Property Inventory. This list of his/her belongings will be reviewed with the patient and the patient will need to sign this form. The hospital is not responsible for lost, stolen or damaged articles listed under the “Items retained by the patient” section of the form.
What should I expect from the admission process?
Upon entering the hospital lobby you will be greeted by the receptionist or and escorted to an the Assessment & Referral lobby area. We will ask you to complete a few pieces of paperwork similar to a doctor’s office visit. An admission counselor will meet with you and explain the assessment and admission process, and a financial counselor will explain your benefits and how they fit with our programs.
At this time, we will ask you questions and complete a full psychosocial assessment, review the programs available and make a recommendation for appropriate treatment. If you need treatment we do not provide, we will provide community resources for you to follow up with at your convenience. Your assessment counselor will discuss the recommendations for a level of care along with programs we offer.
Once you sign the admission paperwork the counselor will go over which items are allowed on the unit and escort you to your treatment unit for orientation with one of our nurses. Patients will be seen by their psychiatrist and an internal medicine physician within 24 hours of admission.
Please bring:
- Form of state or federally issued ID
- Insurance card
- Emergency contact information
- List of current prescription medications
- List of important phone numbers
- Medical Power of Attorney or Guardianship Paperwork, if needed
- Legal documents proving legal guardianship for a minor
How do I obtain a patient ID?
Every patient is protected under the HIPAA (Health Insurance Portability and Accountability Act) law that requires us to keep our patient’s identity confidential.
If you are a referring professional attempting to contact your patient please contact us and ask for one our community liaison’s to provide assistance.
The patient will be given a unique ID number when he/she is admitted. He/she will have the opportunity to give their patient ID number to whomever he/she chooses. In the case you have not received this number please leave a message for the patient and if he/she is admitted to the hospital, our staff will give the patient a message that you are attempting to reach him/her. Receptionists will not be able to confirm if a patient is admitted to the hospital without the patient ID, but if you leave a message and the person you are trying to reach is at the hospital the message will be delivered. If the patient does not want to provide their ID, this is their right and the phone call may not be returned.
We strive to include friends, family and referral sources in the care of our patients, but we do respect the confidentiality of each patient and adhere to HIPAA laws.
What kind of therapy and services will I receive in the hospital?
THERAPEUTIC COMMUNITY
The hospital offers specialty programs. These therapy models allow the opportunity for patients with similar issues to process in a group setting under the care of a psychiatrist
PROVEN, EVIDENCE-BASED THERAPEUTIC APPROACH
Trauma focused Cognitive Behavioral Therapy
Therapy is based on working with the patient in the development and integration of knowledge, skills and process. The healing is accomplished through integration of respect for the patient, family, community, culture and religion. The patient is motivated through active therapy, assignment completion, encouragement, and motivation while supporting the patient through trauma work. Emotional responses to trauma often trigger maladaptive behaviors which may present in aggression, opposition to authority figures or other harmful behaviors. Being in a safe environment while the patient receives feedback and develops healthy coping skills is essential. Key components of therapy includes psych-education, family therapy, relaxation therapy and helping the patient connect the thoughts, feelings and behaviors. The successful outcome results in the patient integrating what has been learned in treatment, how the patient relates to others and what they can expect in the future.
Cognitive Behavioral Therapy
Cognitive Behavioral Therapy (CBT) is a short-term, present oriented, evidenced based therapy used to treat a wide variety of psychiatric disorders and psychological problems, including but not limited to mood disorders and anxiety disorders. CBT is individually tailored in order to build a strong therapeutic alliance and emphasizes collaboration and active participation from the treatment team and the patient. CBT is a time-limited approach to therapy designed to focus on the present time. One of the core values of CBT is to teach patients how to identify, evaluate, and respond to their dysfunctional thoughts, behaviors and beliefs in order to change the individual’s thoughts, mood, and behaviors to be more functional and healthy.
Dialectical Behavioral Therapy
Dialectical Behavior Therapy (DBT) is an active, effective therapy designed to assist the patient to work through major issues and to function to the patient’s potential. DBT has been found to be successful with patients that self harm, have difficulty with relationships and can be successful when other forms of therapy have failed. DBT is a form of CBT designed to teach the patient to develop skills for coping with stress, regulate emotions and improve relationships with others. DBT includes mindfulness, interpersonal effectiveness, emotion regulation, and distress tolerance. Each of these skills have specific coping strategies that are taught to patients in group sessions and is then practiced to promote the transfer of skills to the patient’s everyday life. Practice is essential to DBT. The therapist supports the patient through the change process. The process emphasizes that everything is interconnected. The belief is that change is constant and inevitable. Finally therapy focuses on integration for the patient to be succeed.
Cognitive Processing Therapy
CPT is a form of CBT that assists patients to recover from Post Traumatic Stress Disorder (PTSD). CPT focuses on causes and consequences of traumatic events that produce strong negative emotions that prevent the patient from accurate processing of traumatic memories and the resulting emotions from those events. Because the emotions tend to be overwhelmingly negative and very difficult to cope with the patient tends to avoid these triggers. This avoidance ultimately blocks the recovery process. CPT incorporates trauma specific cognitive techniques designed to assist the patient with progress toward recovery. The primary focus of treatment is to assist the patient to understand the connection of the traumatic event and the maladaptive behaviors. The goal to reduce the ongoing negative effects on the patient. Education is a critical component of the therapy. Identification of the maladaptive beliefs is essential for recovery from the traumatic experiences. Processing the trauma is necessary. Ultimately the goal is to clarify and modify the cognitive disorders. The patient can then utilize newly developed skills in the road to recovery.
Living In Balance
Living in Balance assists patients to address life issues that are often neglected during addiction, work with the Twelve Step Program and improve emotional well-being. The focus is on integrating the patient’s mental health disorder into their addiction treatment program, allowing them to bring their life back into balance. Sessions focus on the effects of alcohol and other drug use on mental health; exploring co-occurring disorders, and education efforts. The building off recovery support systems, development of decision making skills and expanding the ability to cope with chronic diseases and substance abuse is essential to the basic foundation of the program.
Education includes but is not limited to:
- Substance use and mental health disorders, how they interact and how treatment helps;
- combating stigma;
- Adequate family and peer support;
- Advanced relapse prevention strategies; and
- Overcoming challenges.
HOSPITAL SERVICES PROVIDED
Medication Management — The attending psychiatrist will assess, prescribe and supervise each patient’s medication. An internal medicine or family practice provider will see the patient for a history and physical exam within 24 hours of admission.
Case Management — A therapist will be assigned to each patient to assist him/her with coordination of aftercare appointments, family and referring professionals.
Group Therapy — We provide group therapy each day with a licensed therapist. Group therapy can be a powerful experience where patients can learn how to monitor their feelings, thoughts and actions and test them in a safe environment.
Family Therapy — A structured family meeting will be arranged if the patient and treatment team determine a family meeting would have therapeutic benefit.
Recreational Therapy — A certified recreation therapist provides interventions which may include self-expression, stress management, problem solving, resource education, social skills, and journaling and leisure/recreation skills. In addition, we provide music and art therapy with specially trained clinicians.
Psycho-Education Group — Provides patients with valuable information and education which may include diagnosis, medication stabilization, wellness, and behavior management techniques.
Process Group — A therapy session held in a group where patients can share their feelings in a safe environment with peers who may have had similar experiences.
School — Adolescents will attend school Monday through Friday with a teacher available to assist students with their school work. We request parents bring their child’s school work no later than three days after admission.
Will my insurance cover my care? What if I do not have insurance?
The hospital accepts most commercial insurance, managed Medicaid and Medicare plans, Medicaid for patients under 21, Medicare and TRICARE®. If you do not have insurance, contact the intake department at (844) 202-5555.
To speak with a financial counselor, please call (844) 202-5555 and ask for the business office.

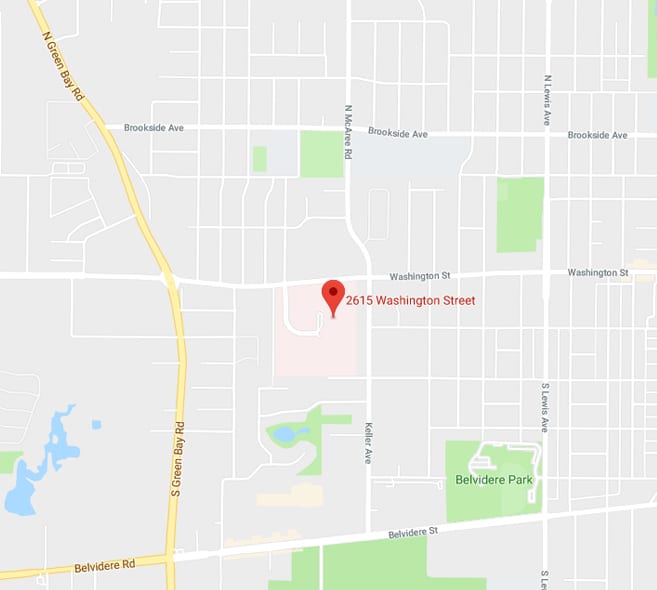
2615 Washington Street
Waukegan, IL 60085
Call Us 24/7 Toll Free:
(855)990-1900
Via I-94 to IL-120 E / Belvidere Rd. in Warren Township.
Take the IL – 120 E / Belvidere Rd. exit from I-94 W.
Continue on Belvidere Rd. Drive to Washington St. in Waukegan.
Lake Behavioral Hospital will be on the right, located at previous Vista Medical Center West campus.